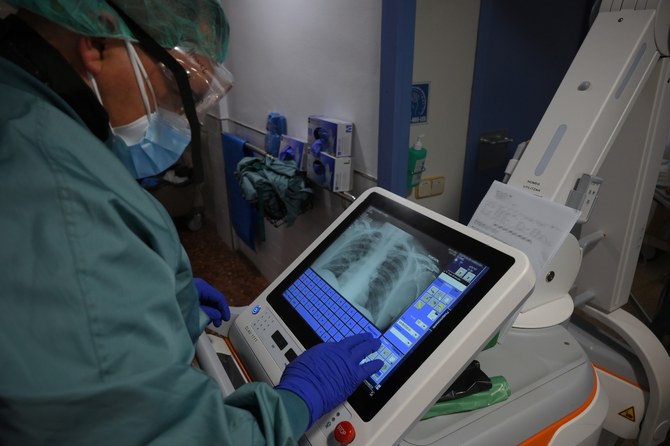
Making every breath count in battle against lung diseases
https://arab.news/gmm4x
Lung health is vital for a long and healthy life, yet too many of us take our lungs for granted. In recent years, the COVID-19 pandemic demonstrated the devastating impact that infectious diseases can have on respiratory systems, yet most common and deadly lung conditions are noncontagious and often inconspicuous. This includes conditions like lung cancer, chronic obstructive pulmonary disease and asthma, which collectively impact millions of people across the Middle East and Africa, with prevalence increasing year on year.
As health ministers from across the world come together this week at the 76th World Health Assembly in Geneva to agree on collective action on global public health, it is essential that more attention is dedicated to lung health. Health policymakers from across the Middle East and Africa owe it to the people and patients in their countries to push for better management of these conditions at the local, national and international levels.
The first step toward addressing this challenge is understanding its magnitude. Lung cancer is the leading cause of cancer deaths worldwide and accounts for more than 100,000 annual deaths in the Middle East and Africa. Since lung cancer is preventable, improving how healthcare systems manage the disease can play a crucial role in decreasing its incidence. Earlier detection is recognized as the best way to reduce the burden of all cancers — but lung cancer is seldom detected early. Shifting detection to an earlier stage could transform lung cancer from a fatal to a treatable condition. Despite a wealth of data to back this up, screening programs are scarce or nonexistent in most countries in the region.
It is crucial to invest in health ecosystems that improve patient outcomes while reducing carbon emissions
Pelin Incesu
Other chronic respiratory diseases, such as asthma, severe asthma and chronic obstructive pulmonary disease, are also a major challenge for health systems across the region and disproportionately affect low and middle-income countries, in part due to limited access to diagnostic tools and treatments. Chronic obstructive pulmonary disease is both preventable and treatable, but in 2019 there were an estimated 10.7 million cases across the Middle East and North Africa, with prevalence growing by 30 percent in the preceding decades, meaning that number is likely now higher. In fact, it is expected to become the leading cause of death worldwide by 2040. In sub-Saharan Africa, this disease has been labeled a “neglected” health problem, with calls for more research to understand the true burden of chronic obstructive pulmonary disease across the continent, so that people living with the condition can get the treatment they need.
The good news is that investment in the prevention, early detection and improved management of lung cancer and other chronic respiratory diseases not only saves lives, but it also makes sense economically. The World Health Organization estimates that, for every dollar spent tackling diseases like this, low and middle-income countries will gain $7 back.
Many lung diseases share common risk factors, such as tobacco use, air pollution, occupational dust and fumes, and exposure to very low or very high temperatures. Building a better understanding among health workers and their patients of these risks and how to avoid or mitigate them should be a priority, especially given the fact that environmental stressors, including climate change, exacerbate many of these challenges, particularly in the Middle East and Africa.
To address this interconnection between lung health and our lived environment, it is crucial to invest in health ecosystems that improve patient outcomes while reducing carbon emissions. Decarbonizing healthcare facilities and patient pathways and adopting energy-efficient practices can help achieve this goal. Harnessing the power of digitalization, artificial intelligence and virtual appointments can also optimize resource use, minimize environmental impact and revolutionize the diagnosis and treatment of lung diseases.
For health systems to be sustainable, they must equip people to be healthy, not just wait to intervene when they are already ill
Pelin Incesu
Moreover, these medical advances also offer new ways to identify and treat lung diseases. For example, many at-risk patients from the Middle East and Africa are now benefiting from new artificial intelligence software that detects lung nodules on chest X-rays in order to flag potential cases for further evaluation. In just a few months, this partnership between Qure.ai and AstraZeneca has completed 30,000 scans across the region, meaning more patients can be identified and begin treatment. Other emerging innovations like mobile lung screening units, synthetic biopsies and precision medicine all have the potential to detect conditions earlier and treat them more rapidly.
Finally, we cannot deliver quality care for our lungs unless we properly equip and educate healthcare professionals, starting at the primary healthcare level. It is only possible for patients to access new technologies when the local health workforce is trained to use them. Collaboration between governments, universities, professional bodies, patient groups and the private sector is essential in this regard, so that the entire healthcare ecosystem is engaged and empowered.
For health systems to be sustainable, they must equip people to be healthy, not just wait to intervene when they are already ill. This shift from sick care to health care could have an untold impact on lung health in the Middle East and Africa and can be achieved by a unified approach to enhancing the prevention, diagnosis and management of lung cancer and other chronic respiratory diseases. By building equitable and resilient health systems, we can make every breath count.
- Pelin Incesu is Area Vice President for the Middle East and Africa for AstraZeneca.